Diabetics: It's fun to say Bionic Pancreas but how about a reality check
 The state of healthcare reporting is just abysmal. It's all link-bait. It's fun to write things like "Random Joe invents cure for diabetes in his garage, saves dying 5 year old." It's surely less fun to read them with you're the one with the disease.
The state of healthcare reporting is just abysmal. It's all link-bait. It's fun to write things like "Random Joe invents cure for diabetes in his garage, saves dying 5 year old." It's surely less fun to read them with you're the one with the disease.
IMPORTANT UPDATE: Scott (me) has now interviewed Dr. Steven Jon Russell, MD, PhD, a member of the Bionic Pancreas Team! Check out their interview at http://hanselminutes.com/431.
It's time for medical journalists to try a little harder and pushback against editors that write headlines optimized for pageviews. The thing is, I've met a dozen General Practitioners who are themselves confused about how diabetes works, and link-bait journalism just ruins it for the public, too. I've received no fewer than 50 personal emails or FB posts from well-meaning friends this last week. "Have you heard? They've cured your diabetes with a bionic pancreas!"
I have been a Type 1 Diabetic for 20 years, I've worn an insulin pump 24 hours a day for the last 15 years (that's over 130,000 hours, in case you're counting), I'm a diabetes off-label body hacker with an A1C of 5.5%. What's that mean to you? I'm not a doctor, but I'm a hell of a good diabetic.
I know what I'm talking about because I'm living it, and living it well. A doctor may be able to tell me to adjust my insulin every 3 months when I see them, but they aren't up with me at 4 am in a hotel in Germany with jet-lag telling me what to do when I'm having a low. Forgive me this hubris, but it comes from 75,000 finger pricks and yes, it hurts every time, and no, my insulin pump doesn't automatically cure me.
Last year the FDA approved an Insulin Pump that shuts off automatically if it detects the wearer is having a low sugar. The press and the company itself called this new feature an "artificial pancreas." Nonsense. It's WAY too early to call this Insulin Pump an Artificial Pancreas.
Now we are seeing a new "bionic" pancreas for which that the press is writing headlines like "A Father Has Invented a Bionic Organ to Save His Son From Type 1 Diabetes" and "Bionic Pancreas" Astonishes Diabetes Researchers."
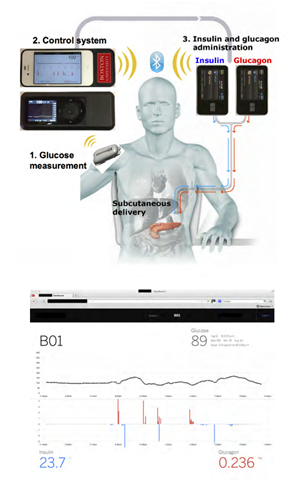
It's a great proof concept for a closed system based on dual insulin pumps (one with glucagon) and a high accuracy CGM managed by an iPhone. But that's a not a fun headline, is it?
"Boston University biomedical engineer Ed Damiano and a team of other researchers published a study earlier this month detailing a system that could prevent these dangerous situations."
Indeed, the study in the New England Journal of Medicine where Ed Damiano, Ph.D. is listed alongside Steven J. Russell, M.D., Ph.D., Firas H. El-Khatib, Ph.D., Manasi Sinha, M.D., M.P.H., Kendra L. Magyar, M.S.N., N.P., Katherine McKeon, M.Eng., Laura G. Goergen, B.S.N., R.N., Courtney Balliro, B.S.N, R.N., Mallory A. Hillard, B.S., David M. Nathan, M.D.
They are clearly all brilliant and of note. Let's break the study down.
"...we compared glycemic control with a wearable, bihormonal, automated, “bionic” pancreas (bionic-pancreas period) with glycemic control with an insulin pump (control period) for 5 days in 20 adults and 32 adolescents with type 1 diabetes mellitus."
They are trying to improve blood sugar control. That means keeping my numbers as "normal" as possible to avoid the nasty side-effects like blindness and amputation in the long-term with highs, and death and coma with lows. The general idea is that since my actual pancreas isn't operating, I'll need another way to get insulin into my system. "Bihormonal" means they are delivering not just insulin, which lowers blood sugar, but also glucagon, which effectively raises blood sugar. They tested this for 5 days on a bunch of people.
"The device consisted of an iPhone 4S (Apple), which ran the control algorithm, and a G4 Platinum continuous glucose monitor (DexCom) connected by a custom hardware interface."
I use a DexCom G4, by the way. It's a lovely device and it gives me an estimate of my blood sugar every 5 minutes by drawing a parallel between what it detects in the interstitial fluid of my own fat and tissues (not my whole blood) and then sends it wirelessly to a handset. I currently then make calculations in my head and decide (Note that keyword: decide) how much insulin to take. I then manually tell my Medtronic Insulin Pump how much insulin to take. The DexCom must be calibrated at least twice daily with a whole blood finger stick. Also, it's not too accurate on day 1, and can be wholly inaccurate after it's listed 7 day effectiveness range. But it's that keyword that this project is trying to help with. Decide. I have to decide, calculate, guess, determine. That's hard for me as an adult. It's near-impossible for an 8 year old. Or an 80-year old. Computers are good at calculating, maybe it can do this tedious work for us.
The thing is, with Type 1 Diabetes there's dozens of other factors to consider. How much did I eat? What did I eat? Am I sick? Does my stomach work? Do I digest slowly? Quickly? Do I have any acetaminophen in my system? Am I going jogging afterwards? Is this insulin going bad? Is the insulin pump's cannula bent, and dozens (I'm sure I could come up with a hundred) of other factors. Read Lane Desborough's paper (PPT as a PDF) on "Applying STPA (System Theoretic Process Analysis) to the Artificial Pancreas for People with Type 1 Diabetes" for a taste of what needs to be done.
The brilliance of this system - this "bionic" pancreas - is this...and these are MY words, no one else's:
The two pump bionic pancreas system gives you rather a LOT of insulin if needed (as if it's descending a plane quickly and dramatically) then it pulls you up nicely with a bit of glucagon (as if the pilot screamed pull up as he noticed the altitude change).
It's the addition of the glucagon to get you out of lows that is interesting. Typically Diabetics have a big syringe of glucagon in the fridge for emergencies. If you're super low - dangerously loopy - your partner can get you out of it with a big bolus of glucagon. But if you put glucagon in an insulin pump, you can deliver tiny amounts and now you are are moving the graph in two directions.
Think I'm kidding about the "pull up, pull up" analogy?
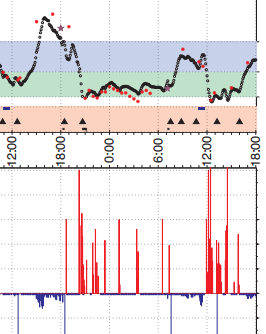
Here's a snippet of a graph from page 15 of one of the Appendices (PDF). Note around 19:00, the blue bar going down, that's a lot of insulin. Then the BG numbers come down, FAST. Note the black triangle at around 20:20. That's "pull up, pull up" and a bolus of glucagon in red. And more, and more, in fact, there are many glucagon boluses keeping the numbers up, presumably happening while the subject sleeps. Then around 07:00 the numbers rise, presumably from the Dawn Effect, and another automatic insulin bolus (an overcorrection) and then more glucagon. It's a wonderfully controlled roller-coaster. This isn't using the word roller-coaster as a pejorative - that is the life I lead as a diabetic.
It's also not mentioned in the press that this system uses lot more insulin than I do today. A lot more, due to it's "dose and correct" algorithm's design.
"Among the other 11 patients, the mean total daily dose of insulin was 50% higher during the bionic-pancreas period than during the control period (P=0.001);"
UPDATE: I spoke to Dr. Russell, and I'm not entirely correct that this system uses a lot more insulin. The system didn't use much more insulin in diabetic kids who have very controlled diets, and was 50% higher in only some of the adults, presumably because (anecdotally) many of them were eating a lot more and "testing" the extents of the system.
I use about 40U a day, total. So we're looking at me using perhaps 60U a day with this system. As with any drug, though, insulin use has its side effects. It can cause fat deposits, scarring at injection sites, and we can become resistant to it. It'd be interesting to think about a study where someone's on 50% more insulin for years. Would that cause increases in any of these side effects? I don't know, but it's an interesting question. Should a closed system also optimize for doing its job with the minimum possible insulin. I optimize for that today, on my own, hoping that it will make a difference in the long run.
But, glucagon isn't pump friendly as it is today. An unfortunate note that isn't covered in any of the press is that they are having to replace the glucagon every day. Juxtapose that with what I do currently with insulin. I keep my pump filled and swap out its contents and cannula (insertion site) every 4-7 days. Insulin itself can surface ~28 days at room temperature although it's most often refrigerated. Changing one of the pumps daily is a bummer, as they point out.
"...the poor stability of currently available glucagon formations necessitated daily replacement of the glucagon in the pump with freshly reconstituted material."
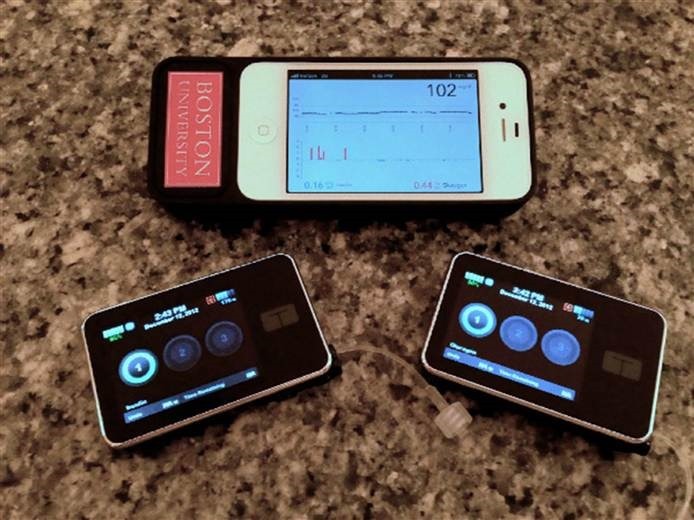
It's early, people. It's not integrated, it's a proof of concept. It's impressive, to be sure, but Rube-Goldbergian in its hardware implementation. Two pumps, a Dexcom G4 inside a docking station, receiving BG data over RF from the transmitter, then the Dexcom wirelessly talking to an iPhone within another docking station.
"Since a single device that integrates all the components of a bionic pancreas is not yet available, we had to rely on wireless connectivity to the insulin and glucagon pumps, which was not completely reliable."
I'm not trying undermine, undercut, or minimize the work, it's super promising, but medical journalists need to seriously understand what's really going on here.
Fast forward a few years, and there will very likely be an bi-hormonal "double" pump with both (more stable) glucagon and insulin that combines with a continuous glucose meter that provides the average Type 1 Diabetic with a reasonable solution to keep their numbers out of imminent danger. Great for kids, a relief for many.
But, just as pumps are today, it'll be USD$5000 to USD$10000. It will require insurance, and equipment, it'll require testing and software, it'll require training, and it won't be - it can't be - perfect. This is a move forward, but it's not a cure. Accept it for what it is, a step in the right direction.
Do I want it? Totally. But, journalists and families of diabetics, let's not overreact or get too ahead of ourselves. Does this mean I should eat crap and the machine will take care of it? No. I'm healthy today because I care to be. I work at it. Every day. As I'm typing now, I know my numbers, my trend-line, and my goal: stay alive another day.
Read my article from 2001 - yes, that's 13 years ago - called One Guy, an Insulin Pump, and 8 PDAs:
"I imagine a world of true digital convergence -- assuming that I won't be cured of diabetes by some biological means in my lifetime -- an implanted pump and glucose sensor, an advanced artificial pancreas. A closed system for diabetics that automatically senses sugar levels and delivers insulin has been the diabetics' holy grail for years. But with the advent of wireless technology and the Internet, my already optimistic vision has brightened. If I had an implanted device with wireless capabilities, it could be in constant contact with my doctor. If the pump failed, it could simultaneously alert me, my doctor, and the local emergency room, downloading my health history in preparation for my visit. If it was running low on insulin, the pump could report its status to my insurance company, and I'd have new insulin delivered to my doorstep the next day. But that's not enough. With Bluetooth coming, why couldn't my [PDA] monitor my newly implanted smart-pump?"
Go an educate yourselves about the "We Are Not Waiting" movement. Hear how Scott Leibrand has a "DIY Artificial Pancreas" that's lowered his girlfriends average blood sugar dramatically using only an DexCom G4 and smart algorithms. You can make a change today, at your own risk, of course.
Read about the The DiabetesMine D-Data ExChange and how non-profit Tidepool is creating open source software and systems to make innovation happen now, rather than waiting for it. Get the code, join the conversation. Exercise, eat better, read, work. You can hack your Diabetes today. #WeAreNotWaiting
Related Links and Writings
- It's WAY too early to call this Insulin Pump an Artificial Pancreas
- The Sad State of Diabetes Technology in 2012
- Scott's Diabetes Explanation: The Airplane Analogy
- YOUTUBE: How my diabetes equipment works
Sponsor: Thanks to friends at RayGun.io. I use their product and LOVE IT. Get notified of your software’s bugs as they happen! Raygun.io has error tracking solutions for every major programming language and platform - Start a free trial in under a minute!
About Scott
Scott Hanselman is a former professor, former Chief Architect in finance, now speaker, consultant, father, diabetic, and Microsoft employee. He is a failed stand-up comic, a cornrower, and a book author.
About Newsletter
Most scientific papers are worthless anyway. But some make for nice media-coverage and that get's them the grants they need to do more research.
Trust me, I have my name on some of those so called peer reviewed papers.
Ideally, future advancements in technology will allow others to stay more in tune with their numbers with minimal effort - which is only way most will have a chance at being as diligent in their tracking.
Glucose and insulin intake are usually modeled using systems of differential equations, which then have to be linearized before a regulator (so the insulin/glucagon pump in question) can be designed. Looking at the high doses of insulin administered by the pump they might be using a very simple (probably proportional) regulator, when a more sophisticated solution (preferably PID regulator) would be suitable.
As a father, Im always looking for answers to my kid disease, Im pretty sure that something has come in the next years and the effort will be rewarded for brave men like you and my son.
Rigth now Im looking for an implant to read glucose levels, I have some info that its been tested on people with good results.
I dream with the day when this days will be remembered as a far away dream.
Thahks for share.
Jose Carlos. .NET Architect in Baja California, Mexico.
ok, A1C 5.5 - this is awesome and I am totally envious. Picking the most important factor to achieving the number, what would it be?
I totally agree with your assessment. 12 yrs ago a pump rep told me their closed loop system is just around the corner.
In my opinion, stable glucagon is a big one that is rarely talked about. As with you, I am looking forward to such a device being commercially available but in the meantime #WeAreNotWaiting.
Thomas
As for my 5.5, I've nailed it twice in a row, so that's about 9 months at that number. I still have highs and lows but I think the #1 thing (number 1, but there are many) is staying at a good number while I sleep. You're unconscious for 8+ hours a day, always have good numbers when you sleep. Don't eat near bedtime and enter sleep at a stable state.
Add to that Ioannidis' findings that over half of medical studies are wrong and the result is quite bleak.
Measuring sugar levels is probably already too far down the change of events so i would guess it's a reactive mechanism.
So just curious if there is a way to measure food intake and predict what the blood sugar will do in future so as to use less insulin and/or prevent the spikes.
From your article i take that you are currently doing it. What am i eating and what will that do after x minutes to my sugar levels. And also what will i be doing in and hour and what blood sugar do i need then to be have enough fuel to do it.
Probably a long way to go and several sensors away before we get near a true bionic system.
It's not just healthcare reporting. It's all reporting. What ends up happening, for me anyway, is I'm completely skeptical of most headlines and articles. I end up trying to find multiple sources about a topic in order to get some level of comfort that the story is accurate. I wonder if the "link-bait" reporting is even easier in healthcare reporting since everybody is always hoping for some "astounding breakthrough" or some "magic" pill that one day comes out of nowhere to cure a disease.
You mention a lot of variables that you personally have to consider when determining how much insulin you are going to deliver. This ranges from the glycemic load of the meal you consumed, your planned physical activity for the new few hours, sensor accuracy, etc.
I'm wondering, without having too much first-hand knowledge since I'm not diabetic, if you could do something with Azure Machine Learning here. What if you could feed your DexCom G4 CGM data into the cloud along with data from an app that computes a glycemic load for your meals, since some carbohydrates are more complex than others and affect blood sugar differently. Combine this with additional data from your FitBit or other fitness activity monitoring device, and have the ML system estimate the optimal amount of insulin to deliver, and hopefully its estimates get better over time as it has a better data set to go off of.
Would something like this be feasible, or does Type I diabetes just vary too much from person to person?
Also how painful it is putting in a new DexCom G4 sensor each week? From your YouTube video it looks a little barbaric. While I'm not diabetic, I do like to see how different foods affect my blood sugar. I currently do the finger prick, but crave more data.
Great article very informative. I heard about this on NPR and then read it a few places. Have to say NPR was hopeful but more realistic in terms of timeline. They do sometime veer very close to unabashed optimism but overall more realistic. It is crazy that this hardware/software costs so much. Hopefully you will one day be able to take advantage of this.
Thanks for all information. I'm also diabetic (for about 25 years). I use insulin pump and CGM (continuous glucose monitoring) for 15 years.
Hope my A1C of will be ever about 5.5% !
Thanks God for modern technologies. I still remember injections made by syrnges with huge needles. For nowaday I don't need anything more (maybe a little bit more self-discipline).
Thanks for inspiration.
But when you say 'don't eat at bedtime and enter sleep at a stable state.' May I ask what do you mean by that? What is a good bs number before bed and what time is your last meal or snack? My son is hypo unaware. Oneendo talked to him like he caused his own diabetes which sent my son into overdrive trying to perfect his numbers.. He's had type 1 for 18 yrs. His highest A1c 's were in the 8's now his A1c's are in the 4.+ range and have been for the last few yrs. Way to low for this worried mom !! Wish his new endo felt the same way. After a few lows and moving back home I find myself encouraging him to have a snack of protein to hold him over during the night .
Lots of respect for you Sir. It is an inspiration.
piece of writing to increase my know-how.
Feel free to surf to my web blog; dentist implants cost Salem Mass
posts. Any wway I will be subscribing to your feeds
and even I achievement you access consistently fast.
Comments are closed.

Living with long term conditions/diseases is tough, you can only look after yourself as best as possible and let the medical guys do the research and maybe one day (probably not in my lifetime) they'll understand my type of epilepsy and be able to cure it without dodgy sounding surgery. Until then I will continue to take the medication, get the right amount of sleep and read medical reporting that is wildly inaccurate and designed to sell copy.. Just like you have described :(