Hacking Diabetes
 NOTE: The top part of this post is background and basics. If you are a diabetic who wants the advanced techniques, they are further down a bit.
NOTE: The top part of this post is background and basics. If you are a diabetic who wants the advanced techniques, they are further down a bit.
Being a Type 1 diabetic sucks. But, if you know anyone who is diabetic then you likely already know that. Over the last twenty years I've tried many different drugs, diets, techniques, and hacks all meant to keep me alive as long as possible. Diabetes is the leading cause of blindness, liver failure, kidney failure and a bunch of other stuff that also sucks. It would be really awesome to die of regular old age rather than some complication of diabetes.
Every few months a diabetic should get a blood test call an hA1c that is a measure of long term blood sugar control. A normal person's A1C is between 4% and 6% which roughly corresponds to a 3 month average blood sugar of between 70 and 120mg/dl, which is great. My A1c has been around 6.0 to 6.7 which is under the American Diabetes Association's recommendation for Type 1 diabetics of 7.0, but not as low as I'd like it.
Related Reading
- The Sad State of Diabetes Technology in 2012
- Scott's Diabetes Explanation: The Airplane Analogy
- YOUTUBE: How my diabetes equipment works
I recently redoubled my efforts and lost about 30lbs, started working out more and removed more carbohydrates by implementing a relaxed paleo diet. This, combined with some medical equipment changes that I discuss below have resulted in my latest A1c - just in last week - of 5.7%. That means for the first time in nearly 20 years I have maintained near-normal blood sugar for at least 3 months.
Basics
A Type 1 diabetic doesn't produce any insulin, and insulin is required to process sugar and deliver it to the cells. Without insulin, you'd die rather quickly. There's no diet, no amount of yoga, green tea or black, herbs or spices that will keep a Type 1 diabetic alive and healthy. Type 1 diabetes is NOT Type 2 diabetes, so I'm not interested in your juicers, raw food diets or possible cures. I've been doing this with some success for the last two decades and I plan to continue - also with success - for the next two.
If you blood sugar gets too high you'll die slowly and rather uncomfortably. If your blood sugar gets too low you'll die rather quickly (or at the very least lose consciousness). The number one goal for a Type 1 Diabetic is to effectively manage insulin and blood sugar levels by simulating a working pancreas where there isn't one. You eat food and your blood sugar rises. You take insulin and your blood sugar lowers. You can prick your finger and check your blood sugar directly then perform some calculations and inject yourself with insulin. If everything works out well then your blood sugar is stable just like a "normal" non-diabetic.
Unfortunately it's never that easy, and in the case of Type 1 diabetes there's a number of factors that complicate things. Sometimes blood sugar rises on its own, sometimes due to illness, hormones, or any of a dozen other factors. The most difficult issue to deal with is that of lag time. When you check your blood sugar you're actually looking at the past. You're seeing your blood sugar in the past, sometimes 15-20 minutes ago. When you take insulin it won't start working for at least 30 minutes, often as long as 60 to 90 minutes. I talk about this in my post Diabetes: The Airplane Analogy. Try flying a plane where your altimeter shows you the past and altitude adjustments are all delayed. I would imagine it's not unlike trying to pilot the Mars Lander. Sadly, there is no such thing as "real time" when it comes to diabetes management.
Basic Management
Basic blood sugar management typically comes down to carb counting and insulin dosage. You'll learn from a Diabetes Educator that your body (everyone is different) will react to insulin in a certain way. You'll learn that, for example, your insulin to carbohydrate ratio might be 1U (1 unit of insulin) to 15g (grams) of carbohydrate. You'll read food labels and if there's a cookie with 30g of carbohydrates or sugars that you'll need to "cover" it with 2U of insulin.
That's the basics. Things quickly get complicated because not all sugars are alike. A cookie with 30g of carbs will "hit you" - or cause a blood sugar rise - much faster than an apple with 30g of carbs or mixed nuts with 30g of carbs. The speed at which carbs hit you is known as the glycemic index of the food. Fruit juices, starches, candy, all have high glycemic indexes.
Why should a diabetic care about how fast food raises their blood sugar? Because the faster your blood sugar moves the hard it is it control. If a cookie can raise blood sugar in 15 minutes but insulin won't start lowering it for an hour you can see how a daily rollercoaster of blood sugar spikes can get out of control.
A reasonably low carb diet makes Type 1 diabetes much easier to handle and manage. I avoid bread, sugar and anything "white." That means no white rice, no white bread, no white sugar. If I'm going to have bread, it'll be whole grain or sprouted wheat.
Portion Size and Cutting Carbs
You should rarely be eating a meal that is larger than your own fist. Better you eat 6 fist-sized meals than 3 giant plates a day. Reasonable portions avoid high sugar spikes.
Cutting carbs is surprisingly easy. I've done personal experiments with hamburgers, for example. A hamburger might require me to take 6U of insulin but that same hamburger minus the top bun was only 3U. It was still satisfying and yummy but that top bun was just empty carbs. That leaves more room for salad (with dressing on the side) which is a diabetic's "free food." You can eat raw veggies until you're bloated and in some cases take no insulin at all, while a Small French Fry could literally set you on a miserable rollercoaster of a day.
Fries and starches are simply off limits. If you eat them, you will pay the price. Pizza, potatoes, tubers of any kind are all effectively raw sugar. Same with all fruit juices and any HFCS (High Fructose Corn Syrup.) In fact, any "-ose" is ill-advised, including Fructose, Glucose and Dextrose.
The Poor Man's Pump
Not that many years ago insulin came in many speed variations. Some were long acting and some short. In recent years we've standardized on two kinds, very long acting where one shot lasts for 24 hours, and fast acting where one shot starts in about an hour and is gone in about four.
We need some insulin running in the background all the time just to stay stable. This is all the basal rate or background insulin. Then when we eat we need a bolus of insulin to "cover" a meal. Long acting insulin can act as the basal and short acting as the bolus.
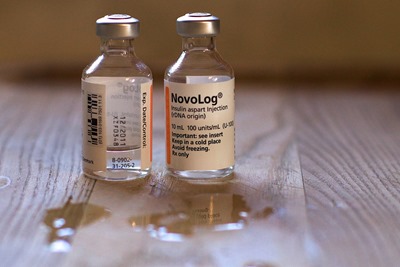
For those that don't have an insulin pump (more on that later) a pump can be simulated by a long acting shot of an insulin like Lantis/Glargene once a day to act as a basal and then short acting insulins like Humalog/Novalog/Apidra for means. You can simulate about 80% of a pump with this "poor man's pump."
Insulin Pumps
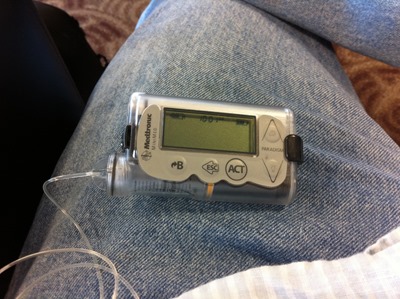 If you've got an insulin pump like I have then you actually have no long acting insulin in you. Instead you've literally got a pump and a tube dripping insulin into your body. I've worn one 24 hours a day, while asleep and awake for over a decade.
If you've got an insulin pump like I have then you actually have no long acting insulin in you. Instead you've literally got a pump and a tube dripping insulin into your body. I've worn one 24 hours a day, while asleep and awake for over a decade.
So where's the basal or background insulin coming from? The pump actually contains only short acting insulin but delivers it in extremely precise and tiny increments all the time. For example, I usually have my pump delivering 0.5U/hr all the time.
Note that none of this is automatic. Pumps are not automatic systems and will only do what you tell them, fortunately or unfortunately. If you're willing to put some thought and effort into it you can do some interesting things with pumps that you simply cannot do with MDI (Multiple Daily Injections.)
Square Wave Basal (Buffet Mode)
One of the things a pump can do that injections simply can't is basal adjustments. Once you've taken a long-acting insulin shot, it's in you and it's going to do its work for 24 hours. The only thing you can do with insulin in you already is add more food or more insulin.
With a pump, though, you can program a either a Square Wave Bolus or a temporary Basal. This can be useful when at an event where you'll be "grazing" and eating little bits over a long period, or in situations where you're eating foods that will take a long time to digest, like pizza.
Temporary basals are also useful for exercise and activity. You can temporarily lower your background insulin for a few hours while you're hiking, for example. Lowering your basal temporarily is your best way to avoid exercise-related lows.
Often Type 1's get into trouble exercising because they'll work out, burn a hundred calories, have a low blood sugar, then eat a few hundred calories thereby negating the original exercise. Lower your basal an hour or so before exercise and set a timer to keep it low for an hour or two. Better an exercise-induced high than an exercised-induced low.
Temporary Basals while crossing Time Zones
I do a lot of international travel and often cross a number of time zones in a single trip as a diabetic. Diabetics on pumps often have multiple basals rates programmed on a schedule and this can cause issues when going overseas.
For example, here's mine:
- 3am - 0.75U/hr
- 8am - 0.5U/hr
- 6pm - 0.6U/hr
- 12am - 0.5U/hr
The 3am to 8am boost there is to manage the blood sugar rise known as the "dawn phenomenon." It's your body trying to get you ready for the day. It's part of your circadian rhythm and it's great for you. It's lousy for me though as it means my blood sugar will just start rising unchecked starting at about 4am.
When travelling, though, what's dawn to me? ;) It takes about a day to adjust for every time zone crossed. So even though I was just in Europe for a week, my "dawn" was slowly moving from the west coast of the US over the Atlantic all week. I needed to be aware of this as I set my pump's clock.
If you change your pump's clock to the destination time zone on the first day, your basals won't reflect your physical reality. You'll get more insulin at 3am local time, for example, but you likely needed it 4 or 7 hour before.
I've found that for simplicity's sake I set my basals while travelling to two 12-hour values, night and day. For example, on this trip I set to 0.6U/hr during the day and 0.5U/hr during the night. This allowed me to see when the dawn rise was happening and deal with it using a bolus, rather than risking a nasty and unexpected low at a seemingly random time. Use temporary basals to smooth things out. I'll set 4 and 6 hour temporary basals as well to "tap it down" or "float up."
Super Bolus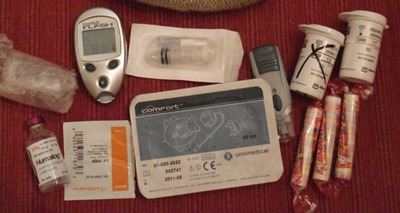
One of the most advanced and most powerful techniques is the Super Bolus. I tend to be a little prejudiced against CDEs (Certified Diabetes Educators) (sorry, friends!) unless they are diabetic themselves. No amount of education can match 24 hours a day, 7 days a week for 20 years. The Super Bolus is one of those techniques that we find after hard work and 3am suffering.
Since even fast-acting insulin often isn't fast enough you'll sometimes want a way to give yourself more insulin now without an unexpected low in 2 to 4 hours.
What you can do is turn off your pump effectively by setting a temporary basal of 0U/hr, and then give yourself the saved amount on top of your planned bolus.
Here's an example. You want to have some ice cream. You take 5U of insulin, your basal is 0.5U/hr. You eat the ice cream and have a bad high sugar in an hour and then a nasty low 3 hours out. The insulin didn't move fast enough to cover the ice cream, and when it did finally start working it took you low because your basal was ongoing.
Instead, you could take 6.5U of insulin and set a 3 hour temporary basal of 0U/hr. You have taken the 1.5U that would have been spread out over 3 hours and instead stacked it on top of the big bolus. The net amount of insulin is the same! You're just clipping that big high and bypassing that nasty low.
You'll need to find numbers that work for you, but the Super Bolus is a powerful technique for avoiding highs and still being able to eat some carbs.
Off-Label Drugs
There are a number of interesting new drugs out for diabetics that aren't super common but if you're interested in hacking your diabetes and you have a willing endocrinologist they could help you.
Symlin is a brand name synthetic amylin and replaces another missing hormone in Type 1 diabetics. Symlin is another shot you would have to take in addition to insulin. We tend to digest food really quickly and that causes nasty post-prandial (after eating) blood sugar spikes. Symlin will slow your digested to that of a normal person and clip those high sugars and allow your insulin to work. Talk to your doctor because it's serious stuff and not to be trifled with. Symlin induced low blood sugars can be really challenging to pull up out of. If you can get past the first two to four weeks of nausea it can be a powerful tool. I took Symlin for a number of years but now I only use it for a few large meals a year like Thanksgiving and Christmas.
Victoza is a new drug for Type 2 diabetics and is explicitly not recommended for Type 1s. However, if your doctor feels it would help you as a Type 1 it can be given "off label." It is a GLP1 inhibitor that also slows absorption of food and its movement through the gut. Finding the right dose can be a challenge, but since Victoza is a daily injectable you can adjust the dose one day at a time.
UPDATE/Correction from Karmel: "Minor point, but Victoza and Bydureon are GLP1 (with a P for glucagon-like peptide) agonists (that is, analogs)-- they mimic the action of GLP1, not inhibit it. Some T2 drugs with similar effects like Januvia are DPP-4 inhibitors, where DPP-4 inhibits GLP1, making a DPP-4 inhibitor a positive regulator of GLP1. But GLP1 we want"
Bydureon has a similar effect to that of Victoza except you take it once a week. It's also a Type 2 drug that is off label for Type 1s. It takes about a month to build up in the system before you see its effects and it can also cause significant nausea.
Order of Food
What a silly heading, but yes, the order you eat can affect your blood sugar. If you drink juice and eat bread before eating a chicken breast your blood sugar will rise faster than if you eat the chicken breast first. If you have a meal with fat in it then eating the fatty part of the meal will slow down whatever comes next. While cheese isn't really good for you, you can slow down the food that comes after it by eating cheese before crackers and an apple, for example.
Lowering A1C by Sleeping
Here's another trick that was so fundamental to getting my A1c down. You're asleep for 6 to 10 hour a day. Nearly a third of your life you're asleep. This is the perfect time to have great blood sugar. There are few feelings worse as a diabetic than waking up after a long night only to discover that you've had high blood sugar all night long. You've been marinating in your own sugar and you didn't even know. What a horrible feeling.
I try not to eat after 8pm so that I have from 8pm until I go to sleep to even out my numbers. You want your numbers to be either normal or heading clearly towards normal as you go to sleep. Just as they say for a good marriage you should never go to bed angry. I say for good A1c results you should never go to bed with bad blood sugar. Even if your numbers are garbage all your waking hours at least try to get them smooth and low as you sleep. Avoid doing anything to move them around after dinner. Eat your dinner, get back to normal, then have a basal rate you can count on and set it for as long as you can.
Equipment
Always be on the lookout for equipment that might allow you to better manage your blood sugar. Sometimes this is covered by insurance, sometimes it's not. It never hurts to ask your insurance company or your doctor.
I've used a Medtronic insulin pump with an integrated CGM for years. It's a good integrated system but the CGM has as considerable lag time showing my blood sugar about 20 minutes in the past. I have also been unimpressed with my OneTouch Mini blood sugar meter. I grow tired of calibrating and coding the meters and I also feel they aren't nearly as accurate as one needs for tight control.
This year I moved from my Medtronic Paradigm Continuous Glucose Meter (CGM) to a Dexcom Seven CGM. I also switched from a OneTouch Mini to a OneTouch Verio.
The OneTouch Verio is a near codeless meter from OneTouch. That means I can just plug in a strip without entering any codes or calibrations. It is rechargeable with a standard mini-USB adapter and it even as a lighted sensor area so you can check your numbers at the movies. (This is a bigger deal than you might realize.)
The Verio, in my opinion, skews high in its readings. When compared to the OneTouch Mini the Verio values are consistently 20mg/dl higher. This is actually a good thing because when calibrated with the Dexcom CGM it nudges me towards an even lower blood sugar goal.
The Dexcom Seven CGM is the single greatest piece of new technology I've ever experience since I was diagnosed at age 20. It's so profoundly amazing and so utterly indispensible I truly can't imagine life without it. It reduced the lag time for my readings from 20 minutes to less than 5. It's far more accurate than the Medtronic and the sensors can stay in for a week or more. It doesn't provide as much historical data as the Medtronic but the accuracy of the Dexcom is a thing to behold. I'm looking forward to the new Animas Vibe with the Dexcom integrated and plan on switching the nanosecond it comes out. Even though the Dexco is yet another thing to carry and keep charged I credit this CGM with helping me get the best A1c test results of my diabetic life thus far.
As with all random blog posts your read on the internet, remember this. I'm not a doctor. I'm just a random dude you don't know. Try all this at your own risk and under your doctor's supervision.
If you'd like to make a tax-deductible donation to the American Diabetes Association and be a part of Team Hanselman, you can donate securely here http://hanselman.com/fightdiabetes/donate. It is appreciated!
About Scott
Scott Hanselman is a former professor, former Chief Architect in finance, now speaker, consultant, father, diabetic, and Microsoft employee. He is a failed stand-up comic, a cornrower, and a book author.
About Newsletter
also - s/never go to be angry/never go to bed angry
With regards to going to bed with as close to normal levels, remember late night exercise can have a delayed affect. To avoid lows in the night make sure you have an understanding of how activity affects your situation. I am not a doctor but in consultation with many others I have found that sticking to a routine until you understand how your body will react - then making minor changes over time to achieve goals while closely monitoring is the safest approach.
All the best - Larry
Thanks for this article. I generally swing by here for .NETty type stuff, but since my wife is currently battling with gestational diabetes, I found this to be interesting. I gave me some good insights and ideas on what to try to get her sugars under control.
Thanks again!
Tim
I'm also glad to hear you like your switch from Medtronic CGM to Dexcom. I'm currently in the process of switching and am very much looking forward to it!
Quick question about your Dexcom experience: Did you run into issues putting it on your belly and potentially sleeping on it? The instructions say be careful and stay away from areas where pressure could be applied. Just curious and certainly looking for more areas than just my waists.
Thanks for the as always wonderful diabetes post and keeping the awareness alive.
Thanks for sharing with me this insight. I had no idea what a diabetic has to go through every day just to survive. I think us non-diabetics could benefit from learning how to eat better.
Bruce
Scott, I decided to NOT get the continuous glucose monitor by watching your YouTube video. The idea of wearing 'Second Skin', it looked unbearable...
It's not only a cumbersome disease, but it's taking a toll on social life and sports too. We often talk about the fact that a non diabetic can't fully understand how it feels physically and emotionally. Without imposing on your personal life Scott, how do you manage it not to get the best of you?
Thanks for taking the time to write this, we both ate every letter of it and no harm was done ;-)
Michel
Brian K
This is the first time I've read an explanation of the Super Bolus...I'm going to have to try it sometime! I definitely struggle with immediate spikes and delayed lows.
It really bugs me that my "sophisticated" One Touch UltraLink communicates wirelessly with my pump...but has no light. Yet my clunky old 1990s glucose monitor had a light lol. I will definitely be looking into this Verio you speak of!
Personally, I struggle with the whole carb counting thing. When they switched me from twice a day injections to basal/bolus, they calculated my lunch to require three units. So far, I've settled at 10 units, occasionally taking 11. Why? Well, it appears that I'm classified as Insulin Resistant, so I tend to break down the insulin as soon as I inject it. Most non-diabetics can get their head round the idea of injections, few can understand that my body kicks in enzymes to destroy the insulin as soon as it hits the blood stream.
Of course, as a type 2, I don't 'need' pumps or continuous monitoring, so I can't get it. Not even if I pay for it. Over here in the UK, I'm lucky in that I get all my meds and test strips for free, but that does tend to mean that I can't get anything other than the basic care. New drugs and expensive equipment just doesn't figure in the budgets.
Still, you manage. You take the pain (and the ugly black spots on the ends of your fingers) and you get on with it. What else are you going to do. This week, I'm off to have my eyes lasered again - I'm in to double figures in both eyes now. The diabetes is manageable, the side effects are a killer!
Cutting carbs is surprisingly easy. I've done personal experiments with hamburgers, for example. A hamburger might require me to take 6U of insulin but that same hamburger minus the top bun was only 3U. It was still satisfying and yummy but that top bun was just empty carbs.
I liked that part :)
In my case, it's the daily salt intake (sodium intake, actually) I have to monitor, both for kidney and bloodpressure well-being (they're closely related anyway). After research, and experimenting, I pretty much came up with the same system: Eliminate the empty-not-so-yummie-just-there-for-filling salty parts, to create space for the yummie parts :)
Burgers work the same way for me: An average bun (or slice of bread) weighs in at around 200mg of sodium (out of max recommended normal intake of 2500mg, for me it should be between 1500 and 2000mg, tops). Remove half the bun, remove half the salt :). As a bonus, you now need less mayonnaise (salty), mustard (salty as hell), and ketchup (salty as hell).
Being creative in these matters goes a long way :)
@Adam
Type 1 has many causes but many common ones are injury (car accident, baseball to the stomach, etc) or serious illness. I'm sure there are piles of other reasons too, just listing the ones I know of that don't include starting as type 2 and failing to control yourself until you nearly die and become type 1.
Thanks a bunch for the information Scott. Even though this doesn't technically apply to me it still does as sugar management is just as important for those who aren't diabetic and aren't interested in becoming type 2.
A friend sent me your posting. I haven't finished reading the whole thing but I wanted to congratulate you on the great score. I understand the A1C struggle. I have a son who battles diabetes. I wish I could trade places with him. As you know diabetes is a slow and deliberate enemy that chips away at you with consistency that can only be battled with the same commitment to consistency. My son is a journalist and I am sure he will appreciate your post. I am going to send it to him to read but I wanted to make sure I took the time to thank and encourage you before the rest of my day managed to rob me of the best intentions.
Scott, keep up the great work both with technology and with your body!
Bayer has a new A1C meter for home.
http://www.a1cnow.com/Our-Products/Patients/A1CNow-SELFCHECK.aspx
There is also a way to convert A1C to eAG, estimated average glucose which is the same units as the daily meter.
http://www.diabetes.org/living-with-diabetes/treatment-and-care/blood-glucose-control/estimated-average-glucose.html
The relationship between A1C and eAG is described by the formula 28.7 X A1C – 46.7 = eAG.
http://professional.diabetes.org/GlucoseCalculator.aspx
Thank you for the article.
David
http://singularityhub.com/2011/01/06/diabetes-defeated-by-a-microchip-silicon-pancreas-to-treat-london-patients-in-2011/
FOOD: If you're eating lower carb, higher protein and/or higher fat meals, you need to figure approximate carbs for those foods, like you would with any carbohydrate. For proteins, my doctor and I worked out (for me) I divide the total grams of protein by 4 to get an approximate amount of carbs to bolus toward. With fats, I use 10% of the total. So 40g of proteins equals 10g of carbs, and 40g of fat is 4g of carbs. Make sure you work with your doctor to figure out protein/fat conversion ratios for you!
And if you're eating high-protein, high fat foots, the conversion to glucose into your bloodstream is much slower than sugars, so you likely shouldn't apply a bolus too soon before or after eating. If I'm eating a low-carb meal, with higher protein and some fat, I typically apply 70-80% of the bolus to start shortly after eating, and then have the remainder start applying over the next hour–this is where having a pump is handy. If you eat a decent amount of carbs, say 40g or more, you're out of low-carb territory and should probably just bolus as normal. Again, work with your doctor to figure out timings and ratios.
Many, many diabetics have gluten sensitivity, despite testing negative for celiac or other markers. I highly recommend giving up gluten for 30 days and see how you feel. This means no bread, pizza, cookies, and a lot of other things. Focus more on lean meats, veggies, healthy fats like olive oil and avocados, and a little fruit.
EXERCISE: Lifting heavy weights typically raises your blood sugar–this surprises a lot of folks. After weights and light cardio, you become MUCH more sensitive to insulin! Be careful. This is because your muscles start to absorb glucose directly to rebuild and repair tissue, whereas before the glucose largely sits in the bloodstream until insulin can be applied. I often decrease my boluses by 40-50% when eating within 30 minutes of working out. That same mechanism is present when you're doing aerobic exercise like riding a bike or running–the GLUT-4 transporters in your tissues activate, and your muscles turn into glucose sinks. That means you need to a) lower you basal rate, which is easy if you have a pump, and b) probably eat periodically to get from hitting lows. When I'm riding my bike, GLUT-4 really turns on after about 30-45 mins of moderate riding. So I turn my basal rate completely off for the duration of the ride and eat about 20g of carbs every 20-30 minutes. Turns out this is a really good eating schedule for cyclists in general, non-diabetic or not.
SLEEP: Depending on your sleep schedule, you might not experience the "dawn phenomenon" that Scott mentions. If you're sleep is in line, you should see it, and likewise, see your blood glucose rise in the morning, in addition to being more insulin resistant for the first part of the day. This is due, among other hormones, to cortisol pumping through you to prep you for activity.
DEHYDRATION and INSULIN RESISTANCE: I haven't looked for any research papers on this, but I've personally found that I seem to be more insulin resistant if I'm not drinking enough water (e.g., I need more insulin than normal, and the speed of insulin takes longer to take effect).
Scott's superbolus is a great trick. With Novolog at least, larger boluses will start taking effect sooner than smaller ones. Something to keep in mind when eating lots of carbohydrates, proteins, fats, or other foods that affect how fast you digest.
I talk about some of this stuff, especially diet, in a post I made last year when I discussed changing my diet to a "paleo" or "ancestral" diet in preparation for a triathlon: http://robbwolf.com/2011/11/18/sean-paleo-type-1-diabetes-endurance/
Fries and starches are simply off limits. If you eat them, you will pay the price. Pizza, potatoes, tubers of any kind are all effectively raw sugar. Same with all fruit juices and any HFCS (High Fructose Corn Syrup.) In fact, any "-ose" is ill-advised, including Fructose, Glucose and Dextrose.
Good advice for everyone, even sans Diabetes.
I recently stumbled across the following video that others in this thread might be appreciate too. Really interesting watch.
"An Organic Chemist's Perspective on Paleo" by Mathieu Lalonde, PhD
http://vimeo.com/27570335
Associated slides are available, but you have to manually click along:
http://www.slideshare.net/ancestralhealth/an-organicchemistss-perspective-on-paleo
I came across Gerson Therapy which claim to solve all types of degenerative diseases (cancer, diabetes etc). The whole therapy believes in Body healing itself. It is quite natural and non-toxic and completely relies on fresh juices and enemas.
Why not just study and try them.
More info :
www.gerson.org
http://gerson.org/gerpress/the-gerson-therapy/
Great article! I've been T1 since 1990. The thing that shocks me the most about being diabetic is the rather absurd inflation. A bottle of Humulin R was $10 when I was a kid, now it's $95. I've never really seen or heard a reasonable explanation for the +800% rise in cost and was wondering if maybe you or anyone else on here has? Also, as there are no true generic versions, people without insurance are pretty much really screwed... and Humulin R is crappy old-school insulin, Humilog and Lantus are almost $200/bottle. How have other people been managing this when most affordable, non employer benefited, independent healthcare options only start to help out after insanely high deductibles?
Thanks,
Marko
Thank you,
Jeanette Collier & Jamie Perez
www
change.org/petitions/revise-names-of-type-1-2-diabetes-to-reflect-the-nature-of-each-disease
What's your take on the latest news out of Boston?
http://www.bostonmagazine.com/health/blog/2013/06/13/boston-childrens-hospital-found-the-root-cause-of-diabetes/
“By identifying the ATP/P2X7R pathway as the early mechanism in the body that fires up an alloimmune response, we found the root cause of diabetes,” says Fiorina. “With the cause identified, we can now focus on treatment options. Everything from drug therapies to transplants that require less immunosuppression is being explored.”
Scott,
Thanq for giving such things which in detail a doctor cant give at a time.really helps.thanq.thanq so much.
But first, full disclosure: I am a cofounder of the company Amylin Pharmaceuticals, I was its first CEO for almost ten years, and I was a member of the research team that pioneered most of our knowledge about the physiology of the hormone amylin. From the day we started that project, two convictions drove our efforts: if Evolution decided that beta cells in all animals should secrete TWO peptide hormones -- insulin and amylin -- there must be a damn good reason for that fact. And, if treating T1D with just insulin remained so difficult six decades after its discovery, perhaps something important was missing. It wasn't easy, but we eventually figured out the reason for the two hormones, and once we understood that, it was obvious why insulin alone is such a difficult drug to use.
I like to use the following analogy to explain how insulin and amylin work together to smooth blood glucose levels. Imagine that your blood pool is a bathtub full of glucose, and mealtime glucose is being turned on at the faucet. The drain of the bathtub is your muscle/fat/liver tissues that take glucose out of the blood pool. At mealtime glucose starts flowing in, so insulin opens the drain by signaling these tissues to take up glucose. If the drain is opened exactly the right amount, the tub glucose remains at a relatively constant level; if the drain is opened too much, the glucose level falls, perhaps to dangerously low levels; if the drain is not opened enough, the glucose level rises, perhaps enough to spill out of the tub.
Now, if you were an engineer designing this system, and you knew that low levels of glucose could be fatal (hypoglycemia) and high levels could be damaging (glycosylation of retinal, kidney, and microvascular tissues), is this how you would do it? Let the mealtime glucose flow in at an uncontrolled rate and focus only on trying to adjust the drain opening to compensate?
Of course not! You would also design a way to control the rate at which glucose flows into the bathtub. Which is exactly what Evolution has done: amylin is the control signal which tells the brain that blood glucose is rising, and in response the brain activates a number of mechanisms to slow down glucose inflow.
Now, why does amylin act through the brain rather than signaling directly to the gastrointestinal system? Because Evolution is smart: if blood glucose levels drop too far, the brain is the first tissue to suffer because it has no internal stores of glucose (it's like a computer without an uninterruptable power supply). So, if the brain detects an uncomfortable drop in blood glucose level, it interrupts the amylin signal to let more glucose into the blood. The brain acts as a "circuit breaker" to prevent the glucose inflow constraints of amylin from leading to hypoglycemia.
Bottom line, amylin cannot cause hypoglycemia because it has no glucose lowering effect when blood glucose drops below normal. In a non-diabetic person amylin cannot induce hypoglycemia.
So, why does the amylin analog, SYMLIN, have an undeserved reputation for CAUSING hypoglycemia? That's an historical accident amplified by continuing ignorance about the interplay between insulin and amylin. When we started the first clinical trials of our amylin analog, the FDA insisted that patients hold their insulin doses constant whether on drug or placebo. The goal was to demonstrate that SYMLIN would have an additive glucose lowering effect to insulin.
Big mistake! The problem was that an appropriate dose of insulin without amylin is much higher than it should be with dual hormone therapy. The initial action of amylin is to slow glucose inflow, but in this context the patient who doesn't back off on insulin is overdosing with insulin; even though the brain pulls its circuit breaker on amylin, blood glucose is falling too fast and hypoglycemia is the result. This effect is similar to what happens in a non-diabetic person who injects insulin: hypoglycemia.
Result: we saw a lot of hypoglycemia adverse events in our first clinical trials. That "tar" has yet to be completely washed off SYMLIN's reputation.
The solution was obvious: when starting dual hormone therapy, titrate the SYMLIN doses upward and the insulin doses downward until the optimal hormonal ratio is achieved. With this approach most patients are able to achieve a comfortable balance at much lower doses of insulin than with insulin alone.
In spite of the initial problems with insulin-induced hypoglycemia, most of our patient volunteers loved the benefits of dual hormone therapy: lower A1c, lower postprandial glucose, less nocturnal hypoglycemia, and WEIGHT LOSS. What was most gratifying is that told us they felt better with SYMLIN aboard.
Anyway, I've probably already lost most readers with this long discussion, so I'll stop here.
So you see, SYMLIN does NOT cause hypoglycemia, insulin does. Sure, it can be tricky getting to the optimal doses, but I know many people who have successfully found their dosing sweet spot. The bigger obstacle to dual hormone therapy is the need for additional mealtime injections.
But that's an engineering problem. The first step will be a dual chamber pump that will supply both insulin and amylin without the extra amylin injections. Longer term, insulin and amylin will be blended together to simulate the correct pancreatic secretion. When these products are available, I predict that hormone therapy of T1D will be much, much easier, and patients will have a better and longer quality of life.
But then, my decades of work in the field have strongly biased me in favor of amylin…
TED GREENE
Comments are closed.
